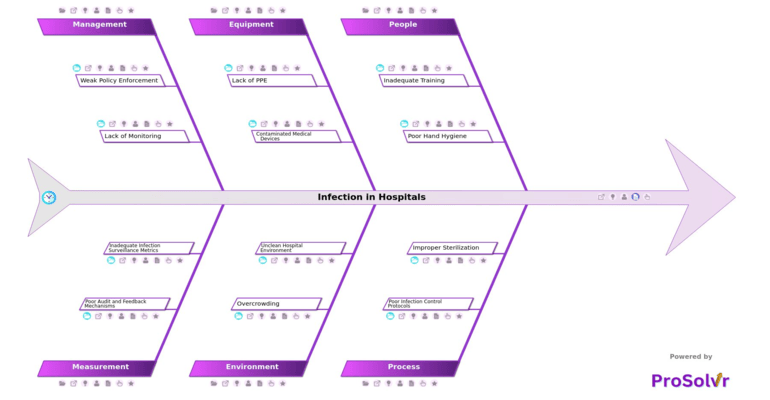
RCA of Infection in Hospitals
Hospital acquired infections are infections that patients get while receiving treatment in a hospital. These infections are not present at the time of admission but develop during the hospital stay. They can affect patients in ICUs, wards, and other areas, and can also spread to healthcare workers. This makes them a serious problem, as they increase patient risk, extend hospital stays, and raise treatment costs.
These infections usually happen because of gaps in people and processes. Poor hand hygiene is one of the main causes, often due to heavy workload, time pressure, or incorrect techniques. Staff may also not receive proper training, especially if there is no structured onboarding or regular updates based on latest guidelines. In many cases, infection control protocols are not clearly defined or not followed consistently across departments. Improper sterilization of instruments and poor separation of sterile and non sterile items can also directly lead to infections.
Equipment and environment also play a major role. Shortage of PPE or poor distribution can lead to unsafe practices. Medical devices may become a source of infection if they are not cleaned properly or are damaged. Overcrowding in hospitals makes it difficult to isolate patients, while shared spaces increase the risk of spread. Unclean environments, especially poorly disinfected high touch surfaces and improper biomedical waste handling, further increase infection risk.
Management and monitoring gaps make it harder to control these infections. Weak enforcement of rules, lack of accountability, and limited supervision reduce compliance. Many hospitals also lack proper systems to track infection data, monitor trends, or conduct regular audits. Root Cause Analysis helps identify these real problems instead of just reacting to infections. ProSolvr supports this with a simple and visual approach using tools like Fishbone diagrams, along with AI driven insights to find deeper causes and create effective Corrective and Preventive Actions. This helps hospitals reduce infections, improve safety, and build a more reliable healthcare system.
Who can learn from the Infection in Hospitals template?
- Healthcare Administrators and Hospital Management: They can strengthen policy enforcement, improve resource allocation (like PPE and staffing), and build accountability frameworks for infection control.
- Doctors and Clinicians: They can better understand how clinical practices—such as adherence to infection control protocols and sterilization standards—directly impact patient safety.
- Nurses and Frontline Healthcare Staff: They play a critical role in day-to-day practices like hand hygiene, patient handling, and use of PPE, making them central to preventing infections.
- Infection Control and Quality Assurance Teams: They can use RCA insights to refine surveillance systems, audits, and compliance monitoring mechanisms across departments.
- Housekeeping and Sanitation Staff: They can improve cleaning practices, especially for high-touch surfaces and waste management, which are vital for controlling environmental contamination.
- Training and Human Resource Professionals: They can design targeted training programs, onboarding modules, and refresher courses to address gaps in infection prevention knowledge and practices.
Why use this template?
Platforms like ProSolvr promote standardization in RCA practices across departments, ensuring that infection-related incidents are analyzed with consistency and rigor. They help teams move beyond surface-level observations and uncover hidden patterns that might otherwise go unnoticed. Over time, this leads to a more proactive approach to infection control, where organizations are better equipped to prevent incidents rather than merely respond to them.
In a healthcare environment where even a minor lapse can have serious consequences, combining structured RCA methodologies with GenAI-powered tools offers a powerful pathway to improving patient safety, operational efficiency, and overall quality of care.
ProSolvr by smartQED to systematically eliminate issues that could cause infections during hospital stay, ensuring holistic healing for the patients.