Improper Disposal of Biomedical Waste
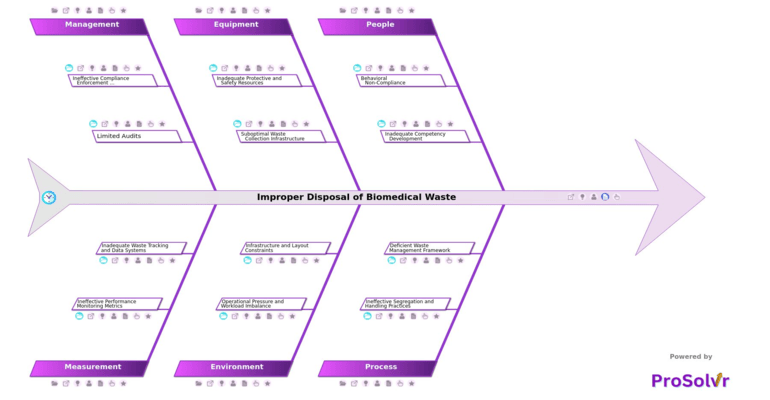
Improper disposal of biomedical waste means not handling or separating medical waste correctly. This includes items like infectious waste, sharps, and medicines. When proper rules are not followed, it can harm healthcare workers, patients, and the public. It can cause infections, injuries like needle stick incidents, and pollution of air, water, and soil. It also increases hospital acquired infections and can lead to legal issues and damage to the organization’s reputation.
These problems usually happen because of gaps in people, processes, and infrastructure. Staff may not follow rules due to low awareness, lack of ownership, or poor training. Sometimes, procedures are outdated or not clearly defined, which leads to incorrect waste segregation during handling, transport, or storage. Poor infrastructure such as wrong bin design, lack of color coding, limited PPE, and bad placement of bins also makes proper disposal difficult, especially when staff are under pressure or workload is high.
Management and monitoring issues make the situation worse. When rules are not strictly enforced and responsibilities are not clear, compliance drops. Lack of proper audits, weak follow up, and poor use of audit results prevent improvement. In addition, when there is no proper system to track waste data or measure performance, it becomes difficult to identify problems or improve processes over time.
Root Cause Analysis helps solve these issues by finding the real reasons behind them instead of just fixing what is visible. ProSolvr supports this by providing a simple and visual way to analyze problems using tools like Fishbone diagrams. It also uses AI to suggest deeper and relevant causes and helps teams create effective Corrective and Preventive Actions. This helps healthcare organizations improve compliance, reduce risks, and ensure better safety for patients and staff.
Who can learn from the Improper Disposal of Biomedical Waste template?
- Healthcare Administrators and Hospital Management: They can identify gaps in policy enforcement, resource allocation, and compliance systems, enabling them to strengthen governance frameworks and ensure adherence to biomedical waste regulations.
- Doctors and Nursing Staff: As primary waste generators, they can improve segregation practices at the source, enhance accountability, and better understand the risks associated with improper disposal.
- Housekeeping and Sanitation Staff: They can gain clarity on proper handling, transportation, and disposal procedures, along with the importance of PPE usage and adherence to safety protocols.
- Infection Control and Quality Assurance Teams: They can leverage the RCA to enhance monitoring systems, design better audit mechanisms, and implement targeted CAPA strategies to reduce contamination risks.
- Training and Human Resource Professionals: They can identify competency gaps and develop structured training programs, refresher sessions, and assessment frameworks tailored to different roles.
- Regulatory Authorities and Compliance Officers: They can use these insights to refine guidelines, improve inspection protocols, and ensure stricter enforcement of biomedical waste management rules.
Why use this template?
By reducing manual effort and cognitive bias, platforms like ProSolvr enable faster, more accurate analysis while maintaining a high level of rigor. Root Cause Analysis provides the methodology to uncover and address these issues at their core, while GenAI-powered solutions elevate this process by making it more efficient, comprehensive, and actionable. Together, they empower healthcare organizations to build safer, more compliant, and resilient waste management systems.
Use ProSolvr by smartQED to effectively root out the causes leading to improper disposal methods, ensuring all round patient safety in healthcare facilities.